What are the Most Common Types of Fungal Infections?
Fungal infections, also known as mycosis, can be contagious as they spread when one comes into contact with an infected person. Since fungi reproduce by releasing spores, the infection can also spread from one person to another. This occurs directly when the fungi are inhaled or when a person comes in contact with disease-causing fungi from infected animals, contaminated soil, or surfaces. Thus, your skin, lungs, and nails are the most likely to get infected.
Some Common Types of Fungal Infection Include

Athlete’s Foot
Athlete’s foot, or tinea pedis, is a type of fungal infection that usually affects the skin on your foot. The infection is caused by four kinds of fungus, all belonging to the group of dermatophytes. The most common one is Trichophyton rubrum.
Causes
The fungi causing athlete's foot can thrive well in warm and moist areas like shoes or socks, making it particularly common among athletes. It is contagious and can spread quickly when one comes in contact with contaminated surfaces while using locker rooms,sports equipment, or public showers. However, it can even infect people living in warmer climates or during the summer months, as the virus can multiply quickly in such environments.
Symptoms
Athletes' foot symptoms may vary slightly from person to person. Some classic symptoms are:
-
Blisters on the affected area
-
Infected skin may be soft, red, discolored, or broken down.
-
Peeling, cracking, or scaly skin
-
Burning, itching, or stinging sensations in the infected area
Diagnosis
By looking at the symptoms on your skin, your medical practitioner may identify an athlete's foot. However, because not all itchy, scaly feet are due to the athlete's foot, your doctor may scrape a small area of the scaling skin and examine it under a microscope to look for the fungus that causes the athlete's foot.
Treatment
Athlete’s foot is treated with several topical over-the-counter (OTC) antifungal ointments, which can be obtained from UK pharmacy. In cases of severe infections, where these medications do not provide relief, your doctor might prescribe additional oral medications as well.
Prevention
Foot care is a must for those infected with athlete’s foot, which means that the feet must be kept clean and dry to help kill the fungus. Give the feet plenty of air to breathe; avoid wearing tight shoes and dirty socks. Wear sandals in locker rooms and public showers.
Is a Fungal infection giving you sleepless nights?
Get in touch with Life Pharmacy and learn about the treatments to cure Athlete's foot.
Jock Itch
Jock itch, or tinea cruris, is another common fungal skin infection that can affect the skin on your genitals, inner thighs, and buttocks.
Causes
Men and boys are more likely to develop this infection, but women and girls can get it too. Like an athlete's foot, jock itch is more prevalent in the summer months and in warm, wet climates. This environment is conducive for the fungi to thrive.
Jock itch is mildly contagious and can spread through direct contact with an infected person. It may also spread indirectly through an object that is carrying the fungus.
Symptoms
-
Redness, itchiness, chafing, irritation, or burning sensation on the groin, buttocks, or thighs
-
Cracking, flaking, or dry peeling skin in the infected area
-
A red, circular rash with raised edges.
Diagnosis
Since jock itch has a peculiar look, doctors usually diagnose it by its appearance. If uncertainty prevails, doctors might opt to inspect the skin sample under the microscope to confirm their diagnosis.
Treatment
Jock itch can usually be treated at home by applying over-the-counter topical antifungal cream, powder, or spray from Online Chemist UK as well as practicing proper hygiene. If the condition is severe and does not improve after two weeks, then it is imperative to consult your doctor. They might give you a prescription cream or stronger antifungal medications.
Prevention
Regardless of treatment, maintaining proper hygiene is critical to preventing jock itch. Changing your clothes, especially your undergarments, is a must to prevent fungal infections. Also, opting for loose-fitting natural fibers like cotton for your underwear can help a great deal. Lastly, avoid sharing items such as towels or sports equipment to avoid contact with those who may have the infection.
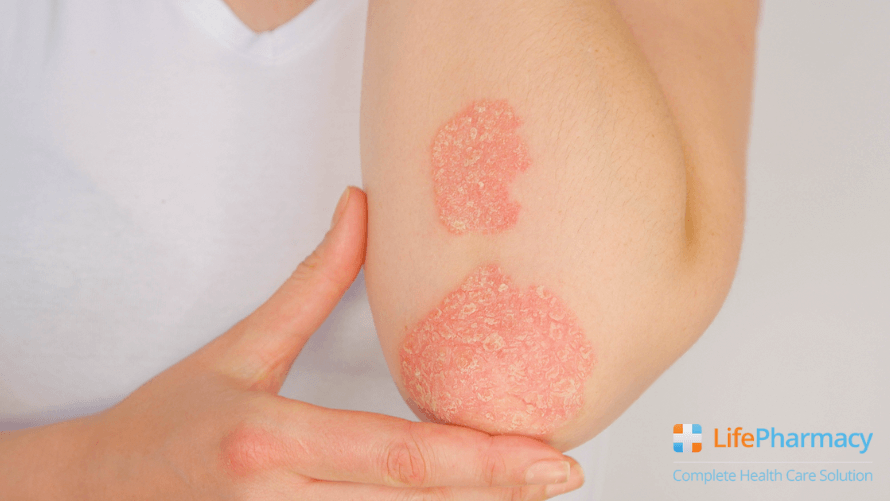
Ringworm
Tinea corporis, also known as ringworm, is a fungus that infects the skin, nails, and scalp. Ringworm is also caused by dermatophytes and thus grows in damp and humid parts of the body. Ringworm is similar to jock itch and athlete’s foot, but when it appears anywhere else on the body, it is called ringworm.
Causes
Ringworm is highly contagious and can spread through direct contact with infected people or pets. The fungus can be spread through objects such as furniture, towels, clothing, and brushes. Since this fungus thrives in soil and mud, people who play or work in such places may contract the infection.
Symptoms
Ringworm usually develops as a red, circular, itchy, and scaly rash. Over time, raised rings may develop around the patch, while the skin in the middle appears normal.
Other signs include:
-
Blistered patches may start to ooze
-
Bald patches on the scalp
-
If it infects the nails, they may appear thick, discolored, or cracked
Diagnosis
Ringworm can be identified by its appearance or after confirming if the patient has come in direct contact with an infected person or animals. Because the fungus glows under a black light, your doctor can confirm its presence by shining the black light over the infected area. A small, scraped skin sample can be sent for lab testing to confirm the diagnosis.
Treatment
Like jock itch and athlete’s foot, one can treat this fungal infection successfully using OTC antifungal creams, sprays, gels, or ointments from Pharmacy Online UK.
Prescription medications to put on your skin or to take by mouth may be recommended in the case of a more severe infection on the nails or scalp.
Prevention
Basic hygiene can help treat and prevent ringworm as well. Keeping the skin clean and dry can help avoid infection. In fact, skin care is indispensable to avoid skin infections. Safety in public includes wearing sandals into public showers or locker rooms. It is imperative to avoid sharing items and towels to keep infection at bay.
Yeast Infections
Yeast infections, or cutaneous candidiasis, are caused by Candida albicans. This is a type of fungus that can infect your skin, mouth, gastrointestinal tract, urinary tract, or genital area.

Causes
These infections aren’t contagious and occur when candida fungus grows out of control. These infections usually occur in body areas such as your armpits and groin, which tend to be warm and moist.
People on antibiotics and those suffering from diabetes or obesity are at a higher risk of contracting this infection.
Infants can suffer from diaper rash due to Candida. It can also cause fungal toenail or mouth infections.
Women are more likely to suffer from vaginal yeast infections. Due to the overgrowth of Candida albicans, the normal balance of bacteria and yeast in the vagina gets disrupted. The cause of bacterial imbalance may be due to either poor eating habits, antibiotics, hormone imbalances, or stress.
Symptoms
Symptoms of a yeast infection on your skin:
-
Rashes are accompanied by itching and burning
-
Pimple-like bumps with patches that may discharge a clear fluid
Symptoms of a yeast infection in your nail beds:
-
Swelling, pain, or pus in the nails
-
A yellow or white nail that detaches from the nail bed
Symptoms of a yeast infection in your mouth (oral thrush):
-
White patches on your tongue or inside your cheeks that are immensely painful
Signs of a vaginal yeast infection include:
-
White or yellow discharge from your vagina
-
Itching, swelling, or burning around the vagina
-
Redness or soreness in the external area of your vagina
Diagnosis
Throat swabs (that look like cotton buds) are usually rubbed against the affected areas to get a sample of the fungi or other microbes that are tested by the lab technicians.
For vaginal yeast infections, doctors may ask about the patient's medical history to rule out the possibility of sexually transmitted infections (STIs). They may also ask whether the patient was recently on antibiotics for any other ailment. They would then examine the vaginal walls and cervix for signs of infection. If needed, sample cells from the vagina would be sent for proper lab diagnosis.
Treatment
Treatment of yeast infections depends on their severity and type:
Oral Thrush can be treated with oral antifungal medications that come in the form of lozenges, pills, or mouthwash that dissolve in your mouth.
In the case of a vaginal yeast infection, your doctor can prescribe antifungal medications that come in the form of creams, pills, or vaginal suppositories.
In cases of severe infections or a weakened immune system, your doctor might recommend anti-yeast medications to be taken by mouth. Your doctor may even suggest probiotics such as Lactobacillus acidophilus to help restore your body’s microbial balance.
Prevention
Avoiding yeast infections begins with a balanced diet and proper hygiene. Wearing loose-fitting clothing made from natural fibers may also help prevent infection. Washing your undergarments in very hot water and changing them often can also help prevent fungal growth.
Conclusion
Fungal infections can be uncomfortable or even painful, and they usually don’t go away without proper treatment. In fact, ignoring the symptoms may cause fungal infections to spread or worsen.
Aside from the aforementioned factors, poor blood circulation, menopause, certain medications or treatments, a weakened immune system, and a nail or skin injury or infection, may all increase your chances of getting a fungal infection. Usually, symptoms such as itchiness, burning, or redness disappear after a few days of treatment, while others like skin discoloration and scaliness last up to a few weeks before healing completely.
Life Pharmacy UK is ready to assist you in fighting these infections and staying healthy. Avail of our round-the-clock services for any of your medical needs.